
Edward Schaeffer, MD, PhD
Director, Polsky Urologic Cancer Institute
Harold Binstein Professor and Chair
Department of Urology
Northwestern University
Feinberg School of Medicine
Four years ago, the Polsky family made a transformational gift to establish the Polsky Urologic Cancer Institute of the Lurie Cancer Center. Thanks to their critical support and vision, we continue to accelerate research efforts and thoughtfully expand diagnosis and treatment options for urologic cancer patients.
From bedside to bench and back again, our researchers seek to develop therapies and search for cures that tangibly impact the lives of real people. We have recruited new scientists and expanded our research team to allow us to continue making groundbreaking clinical discoveries, enroll more patients in clinical trials and advance our world-class research. In partnership with the Lurie Cancer Center, the Department of Urology enrolled more than 600 patients in over 25 clinical trials in 2022.
Clinically, we offer premier diagnostic and treatment capabilities, with the goal of achieving superior results for patients. Northwestern Memorial Hospital is ranked No. 1 in Illinois and has had the top-ranked Urology program in Illinois for 23 consecutive years, according to U.S. News & World Report, 2022 - 2023. Lurie Cancer Center at Northwestern Memorial is ranked once again among the nation’s top 10 Cancer programs, and continues to be the top Cancer program in Illinois. We earn these distinctions by being a leader in innovative research, resulting in the delivery of integrated urologic care that improves the health and quality of life for patients at Northwestern Medicine and beyond.
Our Year in Review highlights our key activities and accomplishments, and the people who made them possible. Together with our patients, scientists and clinicians, we will continue to advance urologic care through research, education and discovery.


Leonidas C. Platanias, MD, PhD
Director, Robert H. Lurie Comprehensive Cancer Center of Northwestern University
Jesse, Sara, Andrew, Abigail, Benjamin and Elizabeth Lurie Professor of Oncology
As a National Cancer Institute (NCI)-designated Comprehensive Cancer Center, Lurie Cancer Center is leading efforts to translate scientific discovery into new and better ways to prevent, diagnose and treat cancer. Guided by our mission, we are providing the highest level of patient-centered care -- informed by research -- and training a new generation of experts to make a lasting impact on the lives of people facing cancer.
We thank the Polsky family for their generous support and Ted Schaeffer for his exemplary leadership of the Polsky Urologic Cancer Institute of the Lurie Cancer Center. By facilitating innovation and collaborative science, we are accelerating life changing advances in urologic cancer research and care.


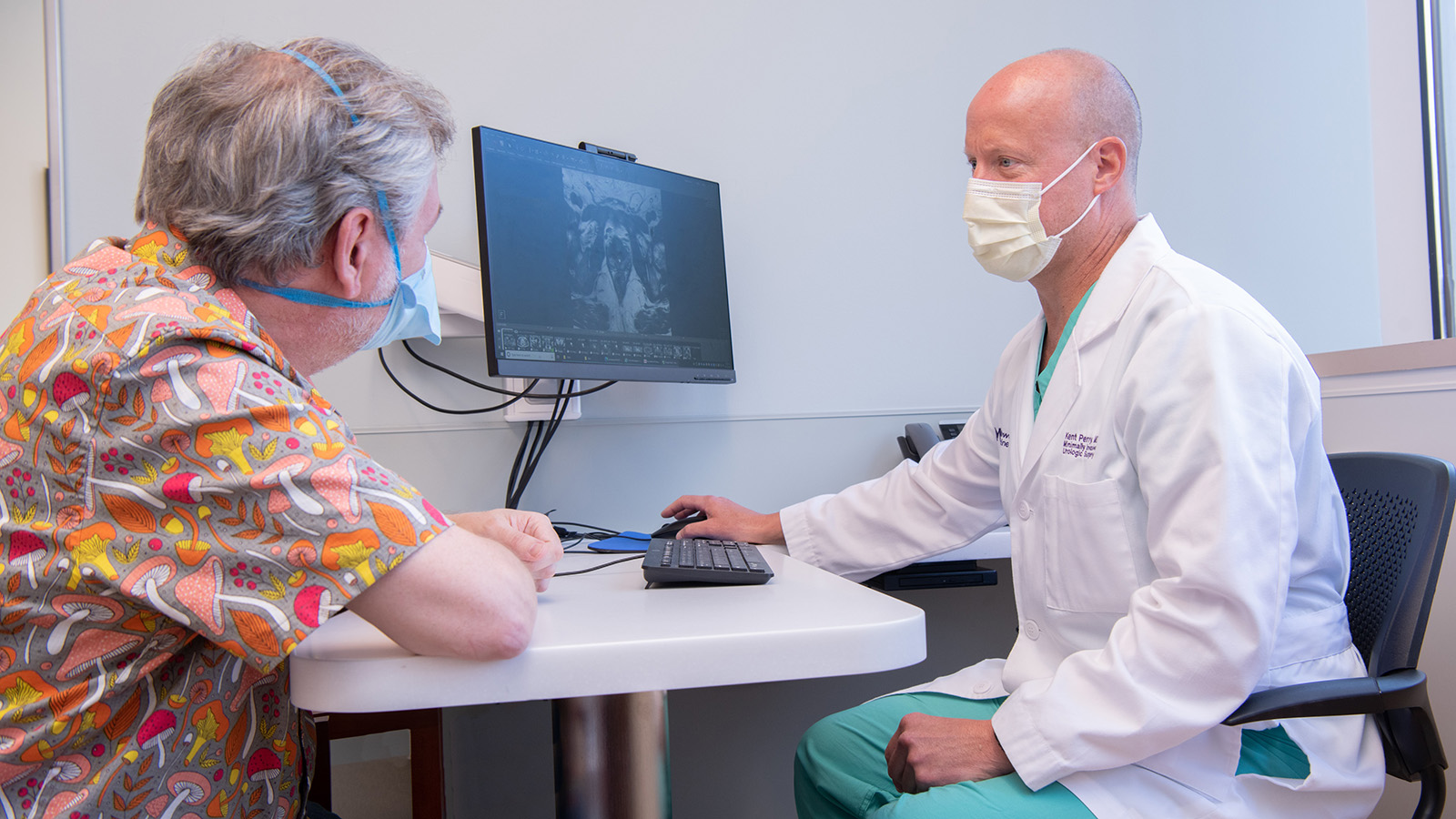
The Polsky Urologic Cancer Institute of the Lurie Cancer Center offers innovative, multidisciplinary treatment of all genitourinary cancers through a disease centric program of research, education and discovery.

 Dr. Patel joins Northwestern as Assistant Professor of Urology. He is an expert in the diagnosis and management of prostate, kidney, testicular and bladder cancer. His specialized research interests include novel diagnostic approaches and optimal surgical management for patients with prostate and kidney cancer. He served on teams at the Johns Hopkins Evidence-Based Practice Center performing systematic reviews that informed American Urological Association guidelines. Dr. Patel also published numerous epidemiologic and comparative effectiveness studies related to renal cell carcinoma, prostate cancer and testicular cancer.
Dr. Patel joins Northwestern as Assistant Professor of Urology. He is an expert in the diagnosis and management of prostate, kidney, testicular and bladder cancer. His specialized research interests include novel diagnostic approaches and optimal surgical management for patients with prostate and kidney cancer. He served on teams at the Johns Hopkins Evidence-Based Practice Center performing systematic reviews that informed American Urological Association guidelines. Dr. Patel also published numerous epidemiologic and comparative effectiveness studies related to renal cell carcinoma, prostate cancer and testicular cancer.
 Dr. Vo is Assistant Professor of Urology with a focus on non-muscle invasive bladder cancer, benign prostatic hyperplasia (BPH) and kidney stones. Dr. Vo is also the Urology Clinical Director of the Northwestern Women’s Bladder Cancer Program. Her academic interests are centered around medical education and improving care for female bladder cancer patients. Dr. Vo completed urology residency at McGaw Medical Center of Northwestern University and earned her medical degree from Northwestern University Feinberg School of Medicine.
Dr. Vo is Assistant Professor of Urology with a focus on non-muscle invasive bladder cancer, benign prostatic hyperplasia (BPH) and kidney stones. Dr. Vo is also the Urology Clinical Director of the Northwestern Women’s Bladder Cancer Program. Her academic interests are centered around medical education and improving care for female bladder cancer patients. Dr. Vo completed urology residency at McGaw Medical Center of Northwestern University and earned her medical degree from Northwestern University Feinberg School of Medicine.
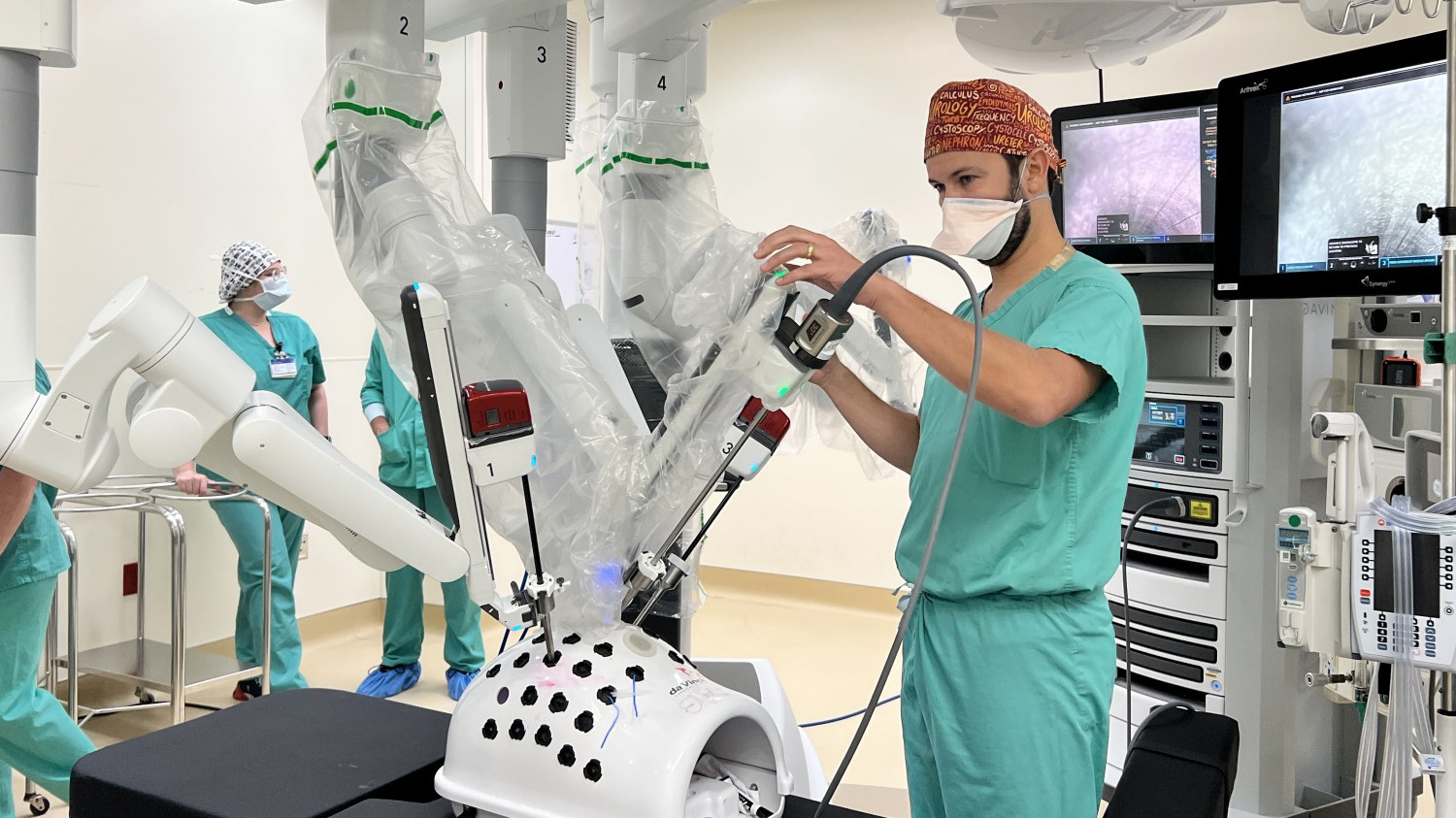
Northwestern Medicine continued its regional expansion and integration with the addition of four new urologists to our regional practices and the opening of the Urology clinic in the Grayslake Outpatient Center. Patients now have access to state-of-the art robotic surgery in all regions with the upgrade of Kishwaukee Hospital surgical robot. According to Ricardo Soares, MD, a urologic oncologist at Kishwaukee Hospital, “The scale of work is way more precise. We will use the technology to treat kidney tumors and remove cancerous prostate tissue.”
Efforts to integrate the Urology service line continue with 2022 bringing enhanced opportunities for collaboration among clinical and administrative teams, allowing NM Urology to leverage knowledge and expertise across the system for the betterment of patient care and increasingly complex clinic operations. The system-wide oncology tumor board offers providers the ability to discuss complex patient care cases and develop treatment options while enabling continuity of care with patients’ community specialists. These efforts support the ultimate goal of enhancing the patient experience from initial contact to on-going follow up. We look forward to carrying the exciting momentum and growth we experienced this year in 2023 and beyond.

Today’s modern approach to scientific discovery involves patients as partners. At the Polsky Urologic Cancer Institute of the Lurie Cancer Center, we always ask: How can we provide even better care to our patients? That may be the question that matters most in advancing urologic cancer care and one that our clinicians and scientists ask each and every day. The stories below highlight our integrated approach to prevention, diagnosis and treatment from experts in all areas of cancer care.
Hiten Patel, MD, Assistant Professor of Urology, specializes in novel diagnostic approaches for small renal masses and treatment options for localized renal masses suspicious for cancer. These approaches and treatments include active surveillance, thermal ablation, radical or partial nephrectomy, and tumor enucleation. "If biopsy is not going to change our ultimate management decision, why would we use it? What we want is a diagnostic approach that adds something to the decision-making process and something that can increase our certainty in making a benign tumor diagnosis," said Dr. Patel.
In this podcast, Dr. Patel discusses how to use novel imaging to augment biopsy to improve tumor identification.
Mara Markzon, LCSW, a clinical social worker in the Department of Urology, specializes in discharge planning for patients undergoing complex urologic procedures. Mara partners with patients undergoing complex surgery, such as cystectomy for bladder cancer, prior to surgery to ensure patients know what to expect post-operatively. Mara evaluates patient resources before surgery and facilitates post-op care and support when necessary. As a result of this discharge planning project, length of hospital stay decreased from 5.6 days to 4.2 days for patients undergoing complex urologic surgery.
In this video, Mara shares her approach to discharge planning, how this approach has improved patient flow and reduced hospital length of stay/time to discharge and how physicians can help facilitate the discharge planning process.
Patients receiving radiotherapy to treat high-risk prostate cancer also benefit from androgen deprivation therapy. The ideal duration of treatment may be roughly two years if receiving external beam radiation and one year if receiving external beam radiation with a brachytherapy boost, according to a study published in JAMA Oncology.
The use of androgen deprivation therapy (ADT) combined with radiation therapy improves cancer outcomes, but comes with significant side effects including effects on the cardiovascular system, mood, lowered libido and loss of muscle mass. This forces clinicians and patients to weight benefits versus costs for use and duration of treatment with ADT, according to Ashley Ross, MD, PhD, Associate Professor of Urology and a co-author of the study. “Determining the optimal balance for length of therapy is paramount,” said Ross, who is also the Clinical Director of the Polsky Institute.
“For men with high-risk non-metastatic prostate cancer receiving radiation therapy, the optimal length of androgen deprivation is likely over 18 months,” Ross said. “Further research to better risk stratify subsets of men with high risk prostate cancer and identify tumors that might be more sensitive to radiation or ADT is ongoing and will lead to more individualized therapeutic regimens that balance cancer control with overall morbidity and quality of life.”
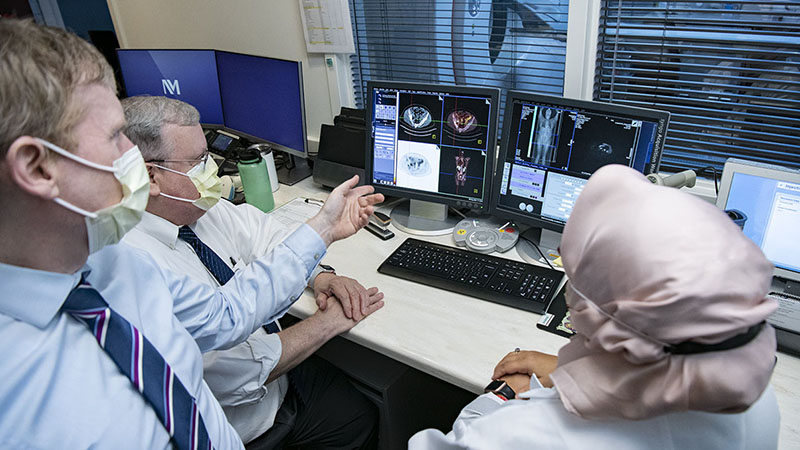
Multidimensional, highly transformative research within the Polsky Urologic Cancer Institute of the Lurie Cancer Center aims to translate scientific discoveries into impactful medical solutions for patients.
 We are thrilled to welcome Rendong Yang, PhD, to Northwestern and the Lurie Cancer Center. Dr. Yang is an associate professor of Urology and principal investigator of the Yang Laboratory at Northwestern University. This lab integrates large-scale, multi-dimensional genomic data to understand the initiation and progression of diseases and drive innovations in precision oncology.
We are thrilled to welcome Rendong Yang, PhD, to Northwestern and the Lurie Cancer Center. Dr. Yang is an associate professor of Urology and principal investigator of the Yang Laboratory at Northwestern University. This lab integrates large-scale, multi-dimensional genomic data to understand the initiation and progression of diseases and drive innovations in precision oncology.
Learn more about the Yang Laboratory
Our scientists are working to drive breakthroughs in treatment and accelerate new discoveries in the field of urologic oncology. Below are some of our team’s transformative breakthroughs in urologic cancer research.

A new drug, administered in combination with standard androgen-deprivation therapy and docetaxel chemotherapy, increased survival in patients with metastatic hormone-sensitive prostate cancer, according to a trial published in The New England Journal of Medicine (NEJM).
This represents a new strategy for managing metastatic hormone-sensitive prostate cancer (mHSPC), according to Maha Hussain, MD, the Genevieve E. Teuton Professor of Medicine in the Division of Hematology and Oncology, a co-author of the study and study steering committee member.
“This is a combination therapy in the first-line for patients with metastatic prostate cancer,” said Hussain, who is also deputy director of the Lurie Cancer Center and a Polsky Urologic Cancer Institute Advisory Board Member.

Polsky Urologic Cancer Institute investigators have identified a gene that confers resistance to a common prostate cancer treatment, according to a study published in Cancer Research.
Targeting the pathway downstream from this gene could reverse therapeutic resistance and improve outcomes for patients with prostate cancer, according to Sarki Abdulkadir, MD, PhD, the John T. Grayhack, MD, Professor of Urological Research, vice chair for research in the Department of Urology and senior author of the study.
“We need to address the issue of therapy resistance, as it may become a larger problem in the future,” said Abdulkadir.

Erdafitinib (balversa), an oral pan-fibroblast growth factor receptor (FGFR) 1-4 inhibitor, is being used in one of the first biomarker-directed trials of high-risk non-muscle-invasive bladder cancer (NMIBC). The Thor-2 trial (NCT04172675) targets tumors with driver mutations in the FGFR3 gene. This gene is altered in 40% to 70% of early-stage bladder cancers and may be a rare driver mutation in bladder cancer. If successful, Erdafitinib would the first precision therapy for early-stage bladder cancer.
In this podcast episode, lead investigator Joshua J. Meeks, MD, PhD, explains the Thor-2 trial and how it could be a new paradigm in bladder oncology.
An epigenetics drug currently being used for the treatment of blood cancers and rare sarcomas can stop the growth of bladder cancer by activating the immune system, reports a new Polsky Urologic Cancer Institute study done in mice.
Published in Science Advances, it is the first time a drug used in hematologic malignancies and rare sarcomas has been used to treat one of the most common solid tumors. The drug, tazemetostat, was originally developed to treat lymphoma.
“We’ve discovered for the first time that the drug actually works by activating the immune system, not just by inhibiting the tumor. We think the specific mutations that may make the drug successful are found in almost 70% of bladder cancers,” said lead study author Joshua J. Meeks, MD, PhD, the Edward M. Schaeffer, MD, PhD, Professor of Urology and associate professor of Urology and of Biochemistry and Molecular Genetics.
Read more about the studyAs part of the Lurie Cancer Center, a National Cancer Institute (NCI)-designated Comprehensive Cancer Center, the Polsky Urologic Cancer Institute provides leading-edge clinical trials for patients with genitourinary cancers, many of which are only available at Northwestern Medicine.

Joshua Meeks, MD, PhD, is collaborating with Janssen Pharmaceuticals on a Phase 1 study to determine the risks and benefits of a new medication delivery system for bladder cancer. Based on the type of bladder cancer and previous treatments, patients will be placed into 1 of 4 groups. All patients will receive an investigational drug delivery system, TAR-210, which is placed in the bladder. TAR-210 is a pretzel shaped tube, made from soft plastic, that is about the size of a quarter. Our physicians will place the TAR-210 pretzel-shaped tube into the bladder and it will release a controlled amount of the study medication directly into the bladder. This study will allow physicians and researchers to determine if there is a safe dose that can be used in other bladder cancer studies, evaluate the drug delivery system, and determine how the body responds to the medication.

Investigators at Polsky Urologic Cancer Institute are investigating new ways to accurately diagnose prostate cancer. A new class of diagnostic agents is the prostate-specific membrane antigen (PSMA). Ashley Ross, MD, PhD, has partnered with Blue Earth Diagnostics, to utilize their radioactive imaging agent rhPSMA-7.3 [F-18] which binds to prostate cancer cells to help locate prostate cancer cells. Patients will be given the rhPSMA-7.3 [F-18] radioactive tracer and will undergo a PET/MR scan to determine if the radioactive tracer will detect and identify the severity of the prostate cancer. Once the scan is complete, all men will undergo a prostate biopsy or a radical prostatectomy. The PET MR imaging along with the surgical specimens will be analyzed to determine if the radioactive tracer detects the prostate cancer and stage of disease with accuracy. PSMA PET/MR is a relatively new technology and has shown improvements in initial detection and classification of prostate cancer.

Qi Cao, PhD, was named the Anthony J. Schaeffer, MD Professor of Urology and Joshua Meeks, MD, PhD, was named the inaugural Edward M. Schaeffer, MD, PhD Professor of Urology.
Shilajit Kundu, MD, Professor of Urology and chief of Urologic Oncology was named the inaugural Janice Binstein Professor of Urology. This gift was made by a grateful patient in honor of Dr. Kundu’s commitment to outstanding clinical care and scholarship in the field of urologic oncology.
A named and endowed professorship represents the highest honor a university can bestow upon a faculty member. These titles recognize the most distinguished and productive physicians and scientists, and they help Northwestern continue to recruit and retain leaders in medicine.

Adam Murphy, MD, Assistant Professor of Urology, received a 2022 Lurie Cancer Center Award of Excellence for his commitment to addressing cancer disparities at Lurie Cancer Center and beyond.
Dr. Murphy has participated on the NCI Cancer Moonshot Panel on Biobanking and is now a standing member of the NIH Molecular Cancer Diagnosis and Classification study section. Most recently, he was selected to lead the Equity, Diversity, and Inclusion Education Committee for the National Cancer Center Cancer Prevention Clinical Trial Network. He is also Assistant Director of Community Outreach & Engagement of Robert H. Lurie Comprehensive Cancer Center, Chair of the Diversity in Men’s Health Committee of SPORE in Prostate Cancer, and Member of the Diversity Committee of Northwestern’s Program in Public Health. In these roles, he advises on increasing minority accruals for clinical trials at the Lurie Cancer Center.

The OncoSET (Sequence, Evaluate, Treat) Program was launched in 2015 to take precision medicine to the next level, combining genomic sequencing and sophisticated molecular analysis to identify new, individually tailored treatments and clinical trials for patients whose cancers are resistant to traditional therapies.
VanderWeele, Associate Professor of Medicine in the Division of Hematology-Oncology, will also serve as co-chair of the Lurie Cancer Center OncoSET Molecular Tumor Board alongside a multidisciplinary team of physicians and scientists, including medical, surgical, and radiation oncologists, molecular pathologists, radiologists, and pharmacogenomics experts.
The Polsky Urologic Cancer Institute offers awards to support clinical, laboratory or translational projects with promising potential to advance knowledge and foster new, innovative research in the field of urologic oncology.
Learn more about the awarded projects
We have selected five key projects to receive funding for the 2022 award year:

Sarki Abdulkadir, MD, PhD
Professor of Urology and Pathology
Gary Schiltz, PhD
Research Professor, Center for Molecular Innovation and Drug Discovery and Pharmacology

Joshua Meeks, MD, PhD
Associate Professor of Urology and Biochemistry and Molecular Genetics

Ashley Ross, MD, PhD
Associate Professor of Urology

Rendong Yang, PhD
Associate Professor of Urology

Young Yoo, PhD
Research Assistant Professor of Urology

Sarki Abdulkadir, MD, PhD, received one of four inaugural Class of 2022 TACTICAL (Therapy ACceleration To Intercept CAncer Lethality) Awards from the Prostate Cancer Foundation (PCF). PCF’s $30 million program will support cross-disciplinary pioneering research toward the goal of developing 21st Century therapies for the most life-threatening form of prostate cancer.
Dr. Abdulkadir and Arul Chinnaiyan, MD, PhD, University of Michigan Rogel Cancer Center, are principal investigators of the $4 million grant, “Tactical Approaches to Repress oncogenic Gene Expression in prostatic Tumors (TARGET).” Co-investigators from the Polsky Urologic Cancer Institute and Lurie Cancer Center are Maha Hussain, MD, and Gary Schiltz, PhD. Sarah Fenton, MD, PhD, is the project’s young investigator.
Their team will employ a suite of cutting-edge drug development techniques to develop an effective inhibitor of MYC, a major driver of about 70% of all cancers, including prostate cancer. These agents will be rapidly translated into clinical trial testing and have the potential to benefit a broad population of patients, including all clinical stages of prostate cancer and many types of cancer beyond prostate cancer.

Young Yoo, PhD, also received a Prostate Cancer Foundation Young Investigator’s Award for her proposal titled “Targeting Metabolic Adaptation to Treat TP53-mutated Lethal Prostate Cancer.” A member of the Abdulkadir lab, Yoo has found that TP53-mutated castration-resistant prostate cancers (CRPC) exhibit high levels of asparagine production, and are sensitive to treatments that deplete asparagine. This project will provide insight into the functions of mutant TP53 and asparagine-mediated metabolic reprogramming in the development of CRPC and provide rationale for targeting this pathway as a new avenue to treat lethal prostate cancers with mutant TP53.

Adam Murphy, MD, was awarded a R01 for his proposal “Using Prostate Health Index and MRI in Combination for Cost-effectively Detecting High-Grade Prostate Cancer in Minorities.”
Recent studies highlight significant promise for multi-parametric MRI (MP-MRI) and Prostate Health Index (PHI) in biopsy-naïve men to help ~25% of men avoid unnecessary prostate biopsies while missing few clinically significant prostate cancers. However, there is a need to increase the number of men who can safely avoid biopsy and expand it to Black and Hispanic men. In conjunction with Shilajit Kundu, MD, Murphy will conduct a comparative effectiveness study to identify strategies using PHI & MP-MRI alone, in series, and in parallel to develop race-specific biopsy strategies with PHI & MP-MRI.

Shad Thaxton, MD, PhD, Associate Professor of Urology, was awarded a 2022 V Foundation Translational Award for his application, “Liquid Biopsy to Measure Novel Biomarker of ImmunoMetabolic Cancer Risk (IMCR).” Thaxton seeks to develop a blood test that provides an accurate measure of ongoing cell stress and metabolic changes to gauge an individual’s risk of cancer. Thaxton has already developed tools that enable rapid measurement of signals in certain blood cells attributed to changes in cell stress and metabolism. This study will determine if these signals can be used to quantify cancer risk.
The Lurie Cancer Center Supportive Oncology Program provides emotional and practical support for patients and families coping with the challenges of diagnosis, treatment and recovery. A multidisciplinary team comprised of oncology social workers, psychologists, and dieticians are dedicated to listening and responding to patient concerns, promoting well-being, and treating each individual with respect and compassion. In partnership with the Polsky Institute, the Lurie Cancer Center's social workers provide tailored counseling and resources for our patients with urologic cancers.
 In this podcast, Mandi Buss, LCSW, OSW-C, a clinical social worker in the Supportive Oncology Program at the Lurie Cancer Center and Polsky Urologic Cancer Institute, discusses how the program provides tailored emotional and practical support for patients and families coping with the challenges of cancer diagnosis, treatment and recovery, and how supportive cancer care improves outcomes for patients.
In this podcast, Mandi Buss, LCSW, OSW-C, a clinical social worker in the Supportive Oncology Program at the Lurie Cancer Center and Polsky Urologic Cancer Institute, discusses how the program provides tailored emotional and practical support for patients and families coping with the challenges of cancer diagnosis, treatment and recovery, and how supportive cancer care improves outcomes for patients.

Eight years ago, the detection of bladder cancer during a routine preoperative CT scan changed Ann Mardon’s life in an instant. Instead of preparing for bladder prolapse surgery at Northwestern Memorial Hospital, the grandmother of three had her bladder removed entirely and a neobladder constructed. The closest substitute to a normal bladder, the neobladder allowed Ann, now 71, to continue her full and active lifestyle.
Smokers are three times more likely to develop bladder cancer than non-smokers. However, Ann had never smoked, and she also didn’t fit the profile for any other high risk factors. While very grateful for the lifesaving care she received from urologic surgeon Joshua Meeks, Ann sometimes wonders why her. “I really don’t know the reason why I got this cancer.”
 Dr. Meeks works to answer questions like Ann’s and those of other patients. The Meeks laboratory studies the disease from many angles to achieve one goal: to cure urothelial carcinoma. Delving into the effect of genetic mutations on immune response, they look for new therapies to attack hard to treat metastatic bladder cancer. Identifying precise biomarkers using specific patient tumor cells, they seek to improve treatment to better preserve the bladder and optimize outcomes. Tackling gender differences in bladder cancer, they hope to better understand why the disease is more aggressive in women even though men are more than four times more likely to develop the disease. There remain many unknowns about bladder cancer that motivate the Meeks team to learn more.
Dr. Meeks works to answer questions like Ann’s and those of other patients. The Meeks laboratory studies the disease from many angles to achieve one goal: to cure urothelial carcinoma. Delving into the effect of genetic mutations on immune response, they look for new therapies to attack hard to treat metastatic bladder cancer. Identifying precise biomarkers using specific patient tumor cells, they seek to improve treatment to better preserve the bladder and optimize outcomes. Tackling gender differences in bladder cancer, they hope to better understand why the disease is more aggressive in women even though men are more than four times more likely to develop the disease. There remain many unknowns about bladder cancer that motivate the Meeks team to learn more.
“Research begins when clinical medicine stops,” says Dr. Meeks, a member of the Lurie Cancer Center. “We take the insight we gain from our patients and frame their questions in ways that we can address them in the laboratory and through clinical trials to impact care.”
Further advancing Dr. Meeks’ unique focus on bladder cancer in women, the Polsky Urologic Cancer Institute offers one of the few bladder support programs specifically for women in the country. The all-female group attracts participants from Texas, Washington, DC, and Alaska, to name a few locations.
“It’s an amazing gathering of women, who all have questions,” says Ann, who helps lead the group. “We listen and we share our experiences so that women with bladder cancer can be ‘heard’ and know they are not alone.”
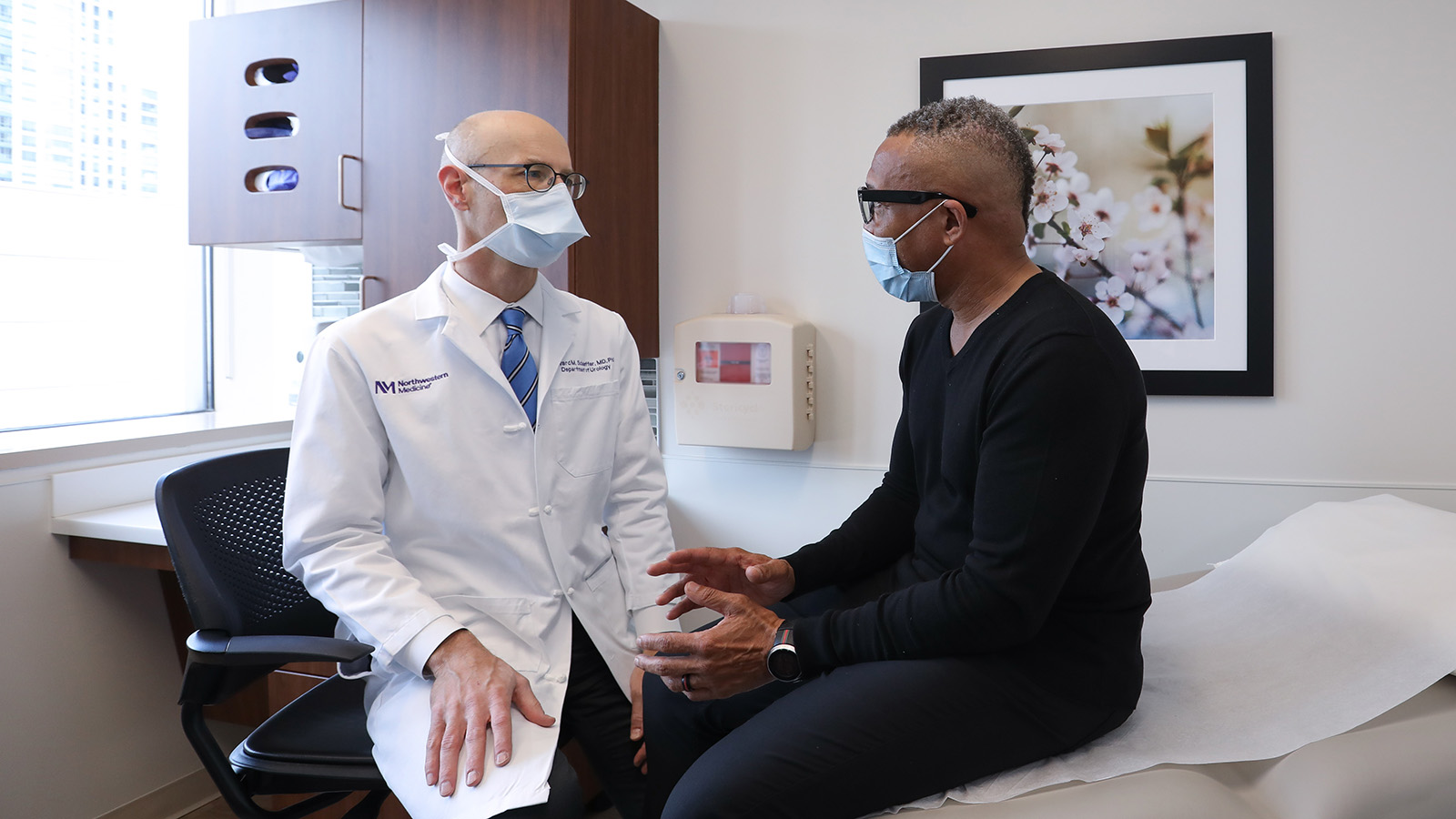
Northwestern and the Polsky Urologic Cancer Institute of the Lurie Cancer Center are committed to fostering a diverse and inclusive environment for faculty, residents, staff, medical students and our patients. Working closely with community partners, we continue to develop initiatives designed to combat health disparities. Recent examples of these efforts are highlighted below.
The Lurie Cancer Center has named Adam B. Murphy, MD, MBA, MSCI, Assistant Director of Community Outreach and Engagement (COE), and Sarki A. Abdulkadir, MD, PhD, Associate Director of Diversity, Equity, and Inclusion (DEI). Murphy will work on initiatives to identify and address cancer disparities across Chicago and beyond. Abdulkadir will lead efforts to enhance the diversity of the research workforce, promote career-enhancing research opportunities for early- and mid-career researchers from diverse backgrounds, and foster an equitable and inclusive environment throughout the Lurie Cancer Center.
The first of its kind in the United States, the Northwestern Medicine Gay and Bisexual Men's Urology Program is designed to deliver better urologic care for patients who were assigned male at birth and identify as gay or bisexual. Channa Amarasekera, MD, Assistant Professor of Urology and Director of the Gay and Bisexual Men's Urology Program, is conducting research on the impact of sexual orientation on treatment decision-making and perceptions of sexual side effects from prostate cancer.
A transformative grant awarded to Northwestern totaling $16 million over five years from the National Institutes of Health (NIH) aims to disrupt systemic barriers that impede the full participation of underrepresented groups by funding the cluster hiring of new faculty in the areas of cancer, cardiovascular, and brain and behavioral sciences.
The five-year grant, along with support from Northwestern, will allow the university to hire 15 new tenure-track faculty, and will deploy innovative strategies to ensure the success of faculty members from historically underrepresented populations. The funding is designed to address the dearth of underrepresented minorities in the life sciences. The initiative aligns with Northwestern’s values, which emphasize the benefits of diversity, equity and inclusion. This overarching initiative, called the Northwestern University Recruitment to Transform Under-Representation and achieve Equity (NURTURE) program is one of only 11 such awards to date in the country.
Learn more about the award
 The Polsky Urologic Cancer Institute offers a variety of educational programs and conferences for the urologic oncology professional. Our programs bring together global leaders in the field of genitourinary oncology to discuss recent developments and advances in the field.
The Polsky Urologic Cancer Institute offers a variety of educational programs and conferences for the urologic oncology professional. Our programs bring together global leaders in the field of genitourinary oncology to discuss recent developments and advances in the field.
The Polsky Urologic Cancer Institute sponsors a free didactic CME lecture series on critical topics in genitourinary oncology titled “Advances and Updates in Urologic Oncology.” With participants from around the world, leaders in urology, medical oncology, pathology and radiology delivered monthly lectures on developments and innovations in urologic cancer care. Topics included robotic reconstruction of complications in urologic oncology, implementation of smoking cessation in urologic oncology practice, and biomarker guided therapy for bladder cancer.
Experts from the Polsky Urologic Cancer Institute represented Lurie Cancer Center on National Comprehensive Cancer Network (NCCN) Guidelines Panels to develop practice guidelines and clinical recommendations used to improve the management of urologic malignancies around the world.

Kidney Cancer Guidelines, NCCN Clinical Guidelines in Oncology
Jeffrey Sosman, MD: Panel Member

Management of Immunotherapy-Related Toxicities, NCCN Clinical Guidelines in Oncology
Jeffrey Sosman, MD: Panel Member

Prostate Cancer Guidelines, NCCN Clinical Guidelines in Oncology
Edward Schaeffer, MD, PhD: Chair

Genetic/Familial High-Risk Assessment: Colorectal, NCCN Clinical Guidelines in Oncology
Brittany Szymaniak, PhD, CGC: Panel Member


Noah Frydenlund and Jenny Guo received the 2022-23 Urology Care Foundation Research Award from the American Urological Association. These awards provide motivated and exceptional urology residents with mentored training to prepare them for careers in urologic research.
Dr. Frydenlund is working under the direction of Joshua Meeks, MD, PhD, to study the molecular features of response to intravesical therapy in stage T1 bladder cancer using digital spatial profiling.
Dr. Guo is working with Amy Krambeck, MD, to evaluate the usage of a mobile health platform for surveillance of kidney stone formers. This is the fourth consecutive year that Northwestern residents have received this award.

These achievements are made possible through the generosity of the Polsky family and other philanthropic partners who help us to further distinguish the Polsky Institute as a leading-edge destination for urologic cancer care and research.
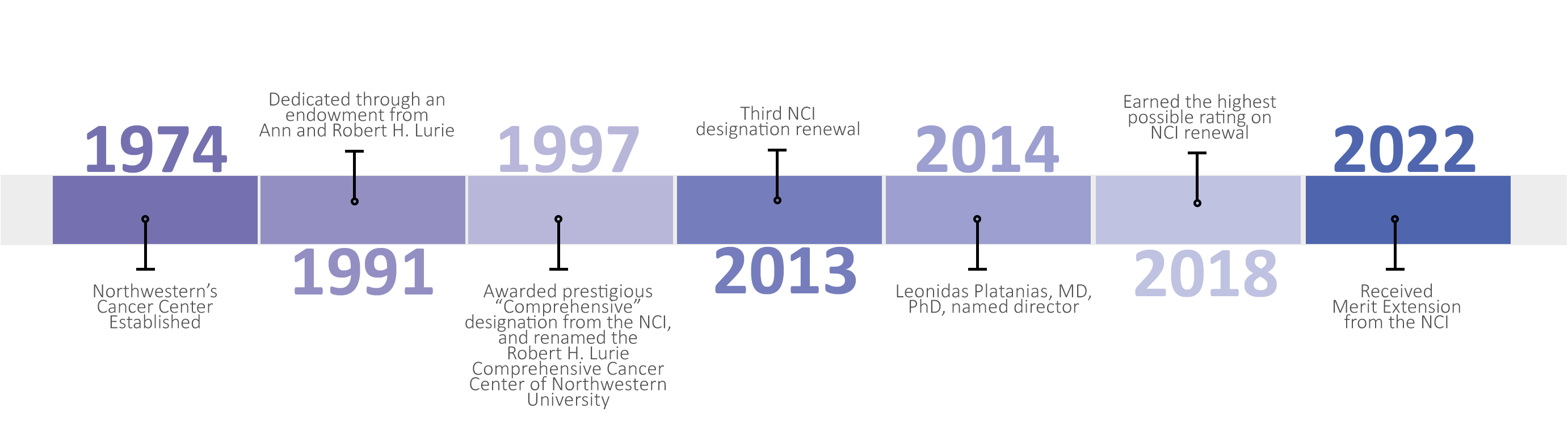
Northwestern’s Cancer Center, founded in 1974, was dedicated in 1991 through an endowment from Ann and Robert H. Lurie. The title was modified in 1997, when the Robert H. Lurie Comprehensive Cancer Center of Northwestern University received the National Cancer Institute’s (NCI) prestigious “Comprehensive” designation, a reflection of our dedication to the highest standards of cancer research, patient care, education and community outreach.
Lurie Cancer Center is a founding member of the National Comprehensive Cancer Network (NCCN), an alliance of 32 of the world's leading cancer centers, devoted to improving the quality and effectiveness of cancer care, and also part of the Big Ten Cancer Research Consortium, a network of academic institutions working together on highly translational clinical trials using the expertise of Big Ten universities.
Through our clinical partnerships with Northwestern Memorial Hospital, Ann & Robert H. Lurie Children’s Hospital of Chicago, Shirley Ryan AbilityLab and the Jesse Brown VA Medical Center, Lurie Cancer Center is uniquely positioned to offer patients leading-edge treatments and exceptional cancer care.

For more information, please visit the
Polsky Urologic Cancer Institute website
Follow Northwestern Urology and Lurie Cancer Center on Twitter



© Robert H. Lurie Comprehensive Cancer Center
of Northwestern University
cancer.northwestern.edu | cancer@northwestern.edu